
Tick bites can be dangerous due to the diseases that ticks carry. Here are tips for tick bite prevention and treatment.
First, what does a tick bite look like?
ADVERTISEMENT
When I lived in Alton NH for 21 years, the place was loaded with the DOG Tick. Had many on me as well as my Beagle. No infections. On my land in VT there were never any ticks until 3 years ago. Then started to find some on me. Not too bad until this past year 2021. In a small fielded area about 1/8 acre between the end of May when I returned to the end of July I pulled 196 off me. Got bit a few times. The previous year being bit I noticed the rash and was treated t the WRJ VA. All was fine. Being bit about 12-15 times I experienced a severe itching and swollen areas anywhere on my body. I scratched vigorously and did draw blood. The VA said I didn't have Lyme via a blood test. Showed the VA Doc the blooded areas. The doc didn't know what caused the itching. Eventually they gave me an antihistamine pill to take once a day. That seem to eliminate the itching. But the other day, 2022 I ran out of those pills and the itching returned. Bought a similar off the shelf and is less effective, but works somewhat. Waiting for the VA prescriptions to arrive. Currently 1500 miles from VT for the winter.
I swear, for the tick numbers encountered, that an airplane flew over and dumped them. In a short time, so many.
I have read about the diseases ticks carry. They bite mice, chipmunks, and other rodents which are known to carry other types of bacteria. That's what I believe I have and I relate the itching being in the nerve system. If a place on one wrist itches, the exact place on the other wrist also will itch at the same time. My VA Doc and perhaps think ticks carry only the Lyme Disease. Baloney. This article mentions attacking the nervous system
My brother in northern VT was bit and he thought it was the flu. Ignored it, got bed ridden and couldn't walk. They carried him to the ST. J hospital. They figured it out and gave him the antibiotics and was cured. The docs there said he was within 2 days of dying.
A new strain has surfaced in Missouri, a guy was bit and died in a week. It serious. The Rocky Mountain Tick carries diseases from rodents there also, prairie dogs, mice, etc. They have had out breaks. The medical people should catch up, treat the problem. Blood tests are important for more than one type of bacteria.
I have done most of the mentioned solutions and hopeful clothing treatments. Each moment I have I look all over my clothing. YET, I'll find them even in bed crawling around. They are reclusive. I have downloaded a lot of info about ticks to see what I'm dealing with. People stay away knowing the / my tick problem.
All the best to all. Hope this helps somewhat.
Taking apple cider vinegar will keep ticks from biting you. I have taken it for years and they don't bite me. They may crawl on me but don't bite. Liquid acv works good but tablets are more convenient for me and work as well as the liquid. If you miss a dose they may bite you so you must use it every day. I believe it also keeps chiggers off and slows down mosqitoes.
Alpha gal is an allergy to all mammalian meat resulting from a lone star tick. It causes severe reactions and/or anaphylactic emergency about 3-4 hours after eating meat. You need to research this allergy to be aware of the side effects and how to live with this. A lot of non mammal foods have natural flavorings that can trigger a reaction. Reading food labels and contacting food companies to know what kind of additives is essential for safe eating. Dining out is a real challenge due to cross contamination. Protect yourself and others from all ticks, because this allergy is becoming more and more widespread.
I live in Heard County Georgia. It is not uncommon to see ticks every day. I try to keep The grass cut as short as I can. There are a lot of oak trees and tall hickory trees and sometimes it seems as if they fall out of the trees. Ticks were not a problem when I grew up as a teen here in the 1970s. The land here is constantly being changed over from hardwoods to Pine. If you look on Google Maps pine farms are being established everywhere. I do not know how it is in other parts of the country but I cannot help but wonder is the pH level of the earth changing and causing these little monsters to be able to inhabit the land more easily. There were not pine forests everywhere back in the 70s.
I have no solution for these ticks I do wear rubber boots.I have family members that live in other parts of Georgia and they are not so far out in the forest as I am, however they experience a lot of ticks too.
I have not been tested for tick disease. However I cannot eat red meat without becoming sick. My daughter was tested for meat allergies and is now allergic to red meat. We have red about alpha gal syndrome and wonder is this what has happened as our neighbor has been diagnosed with it.
If the nymph tick get on (sometimes it’s like a million baby spiders)the best thing to stop them from moving rapidly is to take some type of oil, baby oil olive oil etc. and saturate where the ticks are then they will not be able to move.
I live in the very northeast part of New Jersey, known locally as 'Tick Central". I can't remember how many times I've pulled a tick off of myself. I'm at the point where I'm considering wearing a Seresto collar! On separate occasions after removing a tick I've called my doctor, I've called the local health department, I've called the county extension service, hell, I've even called my dog's vet! No one does tick testing, nor were they able to tell me who does. Gotta love Jersey! Oh, and before anyone suggests using bug repellant, I have a complete arsenal of tried and true concoctions in my hall closet. Thank you.
I spend a lot of time in the woods in East KY where tick populations have exploded over the last decade with the reintroduction of deer and turkey. I have found powdered sulfur, an old time remedy which is a bit more work to apply, and promethrin are most effective.
Ticks never bothered me when I lived in Iowa. My advice was to check for ticks after being outside. Brush your hair and take a shower was my protocol. Ticks then were no big deal. After getting a tick bite behind my knee where the tick embedded for 3 days, I have changed my tune. The tick became the size of a small marble and I was very ill. It was diagnosed as Colorado tick fever. I had all the symptoms outlined in this article. Now my protocol when going outside is to use Ben's Tick Repellent. It repels ticks and also insects like mosquitoes and fleas. I now think that ticks are a big deal!
I've had a tick on me twice, once in Florida, once in NY. No illnesses noted, but it's certainly unpleasant to find them, since they don't hurt when they bite and can be attached to you for a while. However, my dog was diagnosed with Lyme which she acquired before I adopted her and put her on flea and tick prevention. This was upsetting - it didn't have to happen, but for lack of medication. It cost about $500 to treat so far and it should be noted that ticks who carry Lyme also carry other bacterial illnesses that need to be addressed if your dog tests positive. While most dogs beat Lyme on their own, that's no excuse not to use prevention, and dogs who test positive could get sick later in life. For dogs like mine, the infection was taking hold. She had no symptoms but those can happen later. Worse, some dogs go into kidney failure, which is fatal. In 6 months we test her Lyme numbers again and see if the medication worked. It was 30 days of pills, 2 pills, twice daily - not pleasant for human or dog. I have confidence my dog will be OK but it's a lifetime worry, even with the medication. Use prevention! Don't pick ticks off your dog when you can give the dog prevention to stop it from happening in the first place! And you don't squish ticks because you should save them for identification purposes if someone gets sick. Put them in a jar of alcohol.
I'm not clear on why the article tells you to never squish a tick with your fingers? I don't think you could get Lyme disease that way and I have found squeezing them between my fingers is the best way to kill the ones that I sometimes find crawling on my dog.
If you put them in a bowl of water with dishwashing detergent you can see them drown, then flush them or throw in trash. The same works for fleas as well. They do not drown in water unless you add detergent.




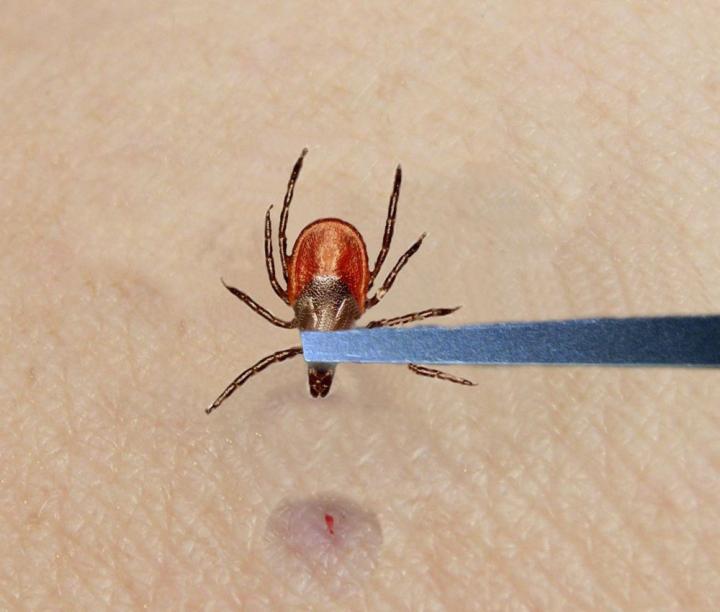 When removing a tick with tweezers, be sure to remove the entire tick and leave no parts in the skin. (Photo Credit: University of Maine.)
When removing a tick with tweezers, be sure to remove the entire tick and leave no parts in the skin. (Photo Credit: University of Maine.) 






